About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

If you find it difficult to understand the subsequent professional descriptions, you can quickly read through this text within two minutes.
Overview of the disease
Knowledge
With the successive identification of oncogenic driver genes in lung cancer, the classification of lung cancer has been further refined from a simple histopathological classification to a molecular classification based on driver genes. EGFR is commonly found in lung adenocarcinoma.
The EGFR gene is a type of gene that expresses epidermal growth factor receptors, promoting normal cell division and proliferation under physiological conditions. However, in some cases, mutations in proto-oncogenes can lead to the development of tumors, with a higher incidence in non-smoking female lung adenocarcinoma. When it was discovered that EGFR mutations often occur in lung adenocarcinoma tumors, people began to consider how to inhibit tumor growth by targeting these mutations. Later, EGFR monoclonal antibodies, commonly known as "targeted drugs," were developed. Typically, EGFR mutations make lung adenocarcinoma more sensitive to specific targeted drugs.
1. The patient's postoperative pathological stage is stage IIIA, which is in the middle-to-late stage. Postoperative targeted therapy was administered without chemotherapy.
2. The presence of lymph node metastases is the main reason for the late postoperative stage, and airspace dissemination and intravascular cancer thrombus are also high-risk factors for future recurrence.
3. NKT therapy utilizes powerful immune cells to eliminate tumor cells that may remain undetected in the body, with essentially no side effects, making it very patient-friendly. NKT cell therapy can be combined with various other treatment options, and long-term stability can be achieved when combined with NKT cell therapy after taking targeted drugs.
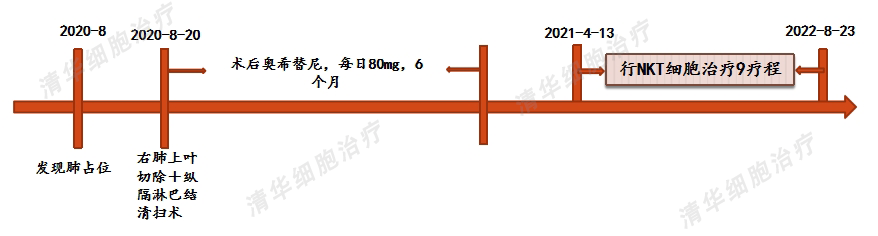
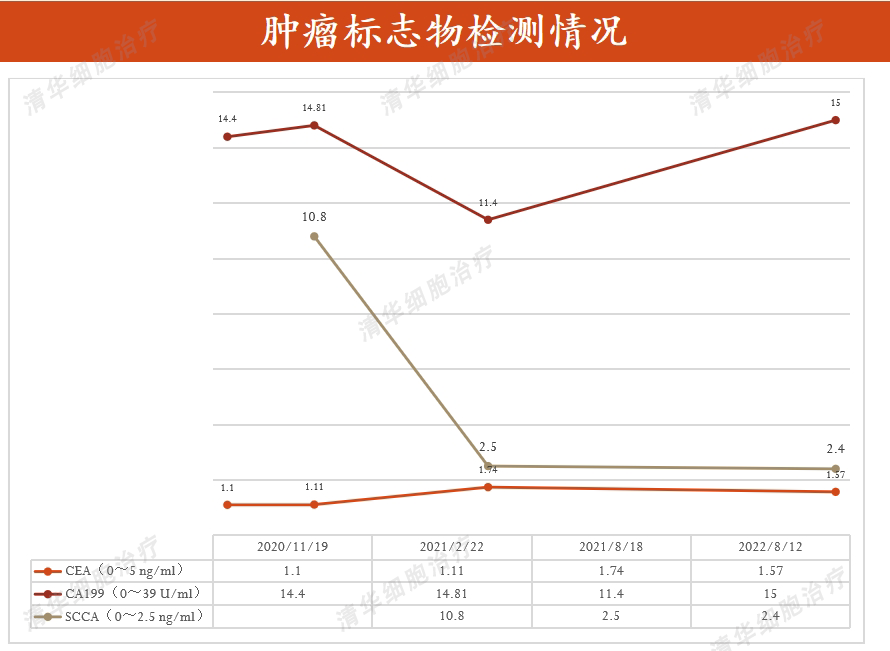
Mr. Zheng decided to undergo NKT cell immunotherapy in April 2021, with an initial plan of one course per two months. Over the course of more than a year, nine courses of treatment were administered, and no signs of recurrence or metastasis were observed during follow-up assessments.
Imaging
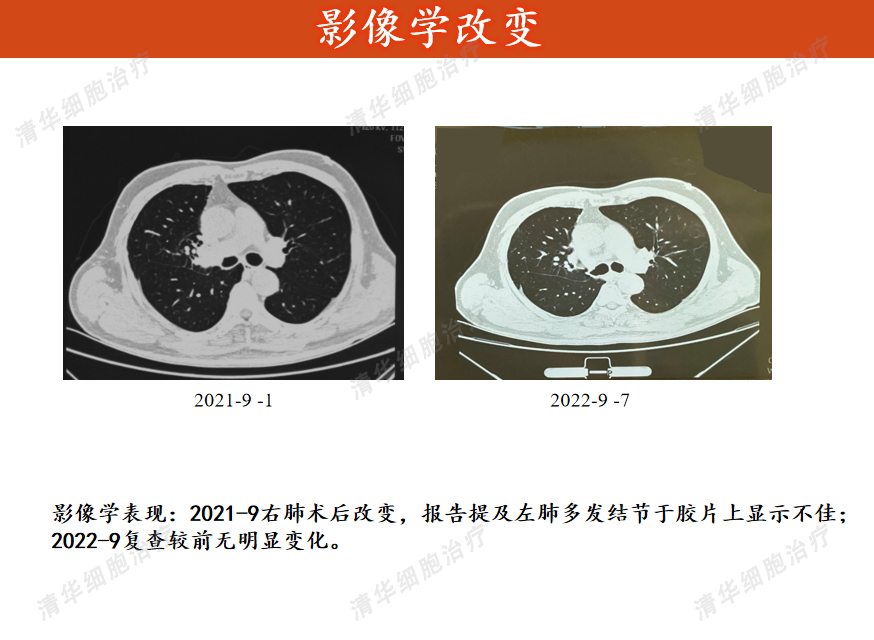
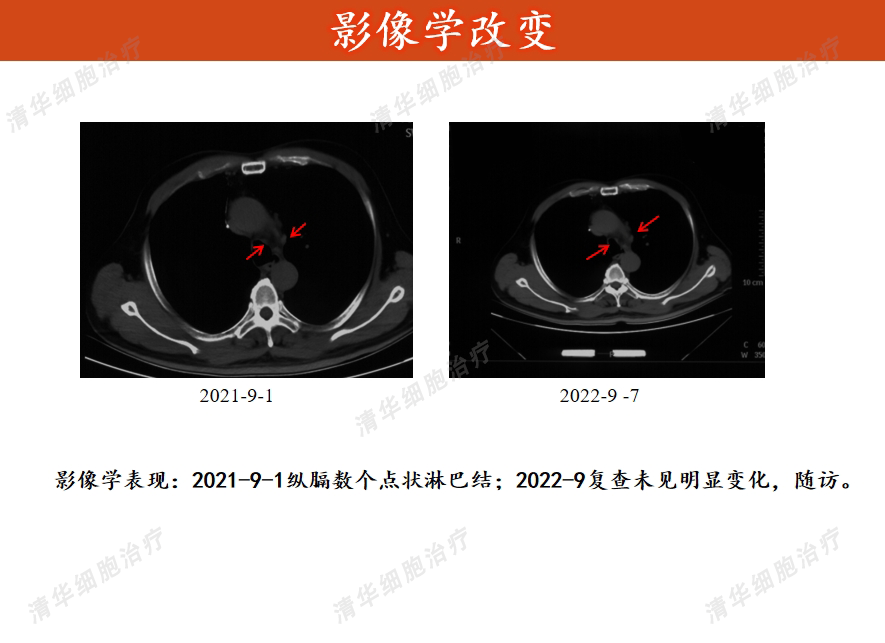
Swelling < H235>
Conclusion and Comments
【1】Wu YL, Tsuboi M, He J, John T, Grohe C, Majem M, Goldman JW, Laktionov K, Kim SW, Kato T, Vu HV, Lu S, Lee KY, Akewanlop C, Yu CJ, de Marinis F, Bonanno L, Domine M, Shepherd FA, Zeng L, Hodge R, Atasoy A, Rukazenkov Y, Herbst RS; ADAURA Investigators. Osimertinib in Resected EGFR-Mutated Non-Small-Cell Lung Cancer. N Engl J Med. 2020 Oct 29; 383 (18): 1711-1723. doi: 10.1056/NEJMoa2027071. Epub 2020 September 19. PMID: 32955177.
[2] Wu S, Luo M, To KKW, Zhang J, Su C, Zhang H, An S, Wang F, Chen D, Fu L. Intercellular transfer of exosomal wild type EGFR triggers osimertinib resistance in non-small cell lung cancer. Mol Cancer. 2021 Jan 18; 20(1):17. doi: 10.1186/s12943-021-01307-9. PMID: 33461557; PMCID: PMC7812728.
Click on the image