About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

If you cannot understand the subsequent professional description, you can finish reading this text in two minutes
Overview of the disease
knowledge
Invasive adenocarcinoma with "multicentric origin"
Although the tumors in Mr. Wang's right upper lung and pleura were both adenocarcinoma in postoperative pathology, the two nodules had different properties, suggesting the possibility of dual primary cancer - that is, having two types of cancer simultaneously, which is a very rare condition. The tumor in the pleura was poorly differentiated adenocarcinoma, indicating a potentially poor prognosis. The degree of differentiation in pathological classification reflects the malignancy of the tumor. Canceration of normal cells generally occurs during the transformation from stem cells to normal cells. The lower the degree of differentiation, the closer the tumor cells are to stem cells and the greater the difference from normal cells, with stronger proliferative capacity, mutation ability, self-repair ability, and resistance to chemotherapy and radiotherapy. Conversely, high differentiation indicates that the tumor cells are more similar to normal cells, which means the malignancy of the tumor is relatively low and the possibility of metastasis is relatively small.
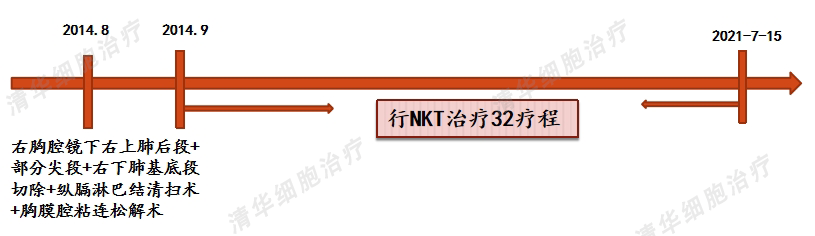
1. The patient underwent radical surgery in the early stage of tumor development, and the postoperative staging was relatively early. Taking targeted drugs for 4 months after surgery had a very positive impact on prognosis, but long-term use of targeted drugs may lead to drug resistance and cannot completely eliminate the risk of recurrence and metastasis.
2. Although the early postoperative staging is good news, the vascular invasion and differentiation type indicated by the pathological results still suggest a high risk of recurrence and metastasis. Even though there are currently no tumors detectable by imaging examination, it cannot be guaranteed that recurrence and metastasis will not occur again.
3. NKT therapy utilizes powerful immune cells to eliminate tumor cells that may remain in the body and are undetectable, and it has basically no side effects, making it very friendly to patients. After completing conventional treatment, NKT cell therapy is used to maintain long-term systemic stability.
Imaging
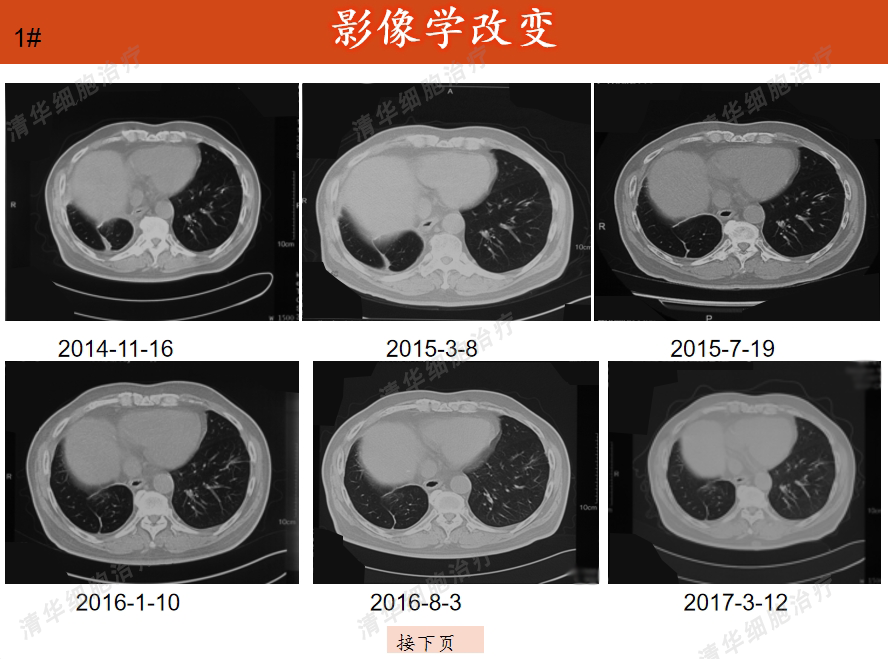
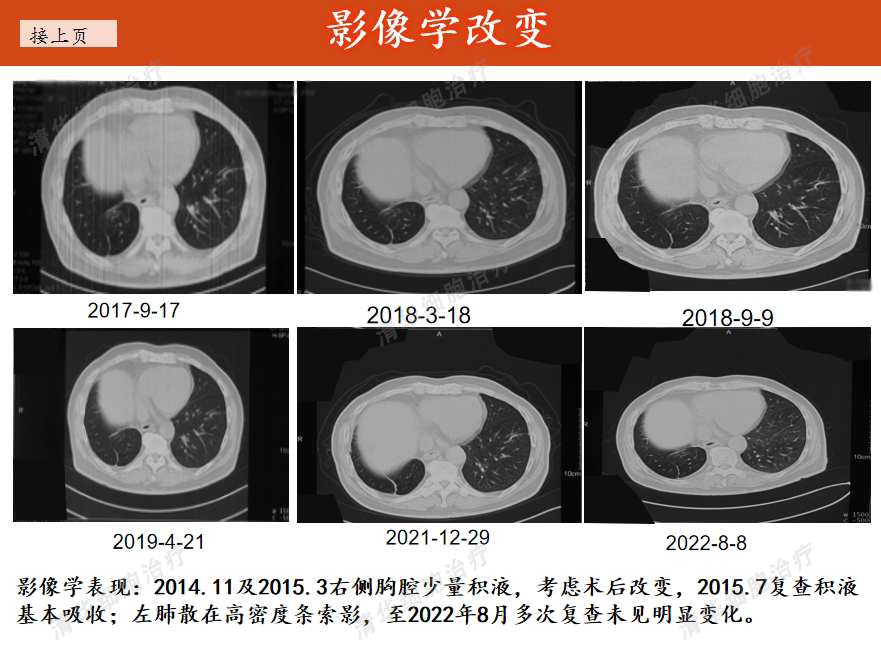
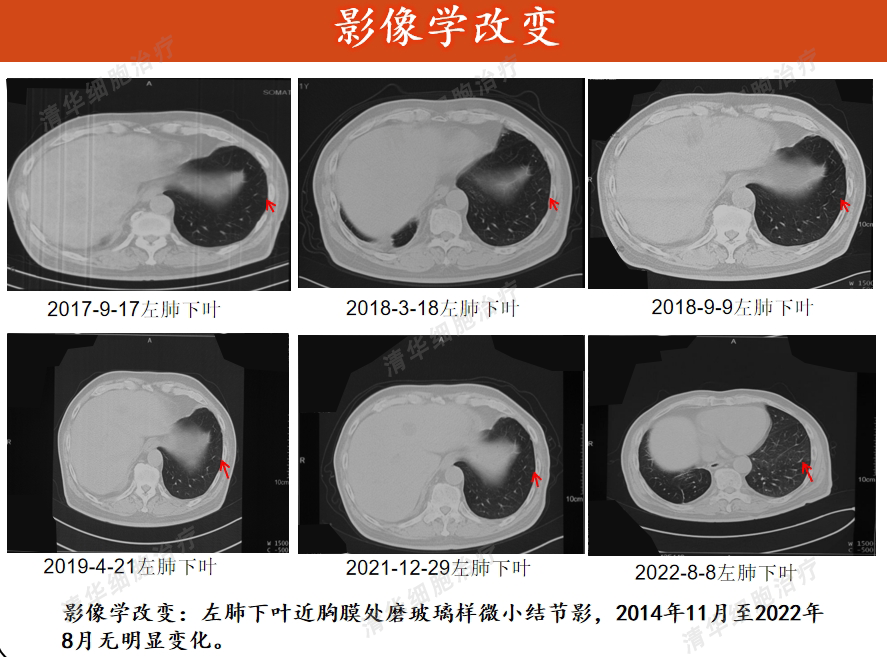
Swelling < H235>
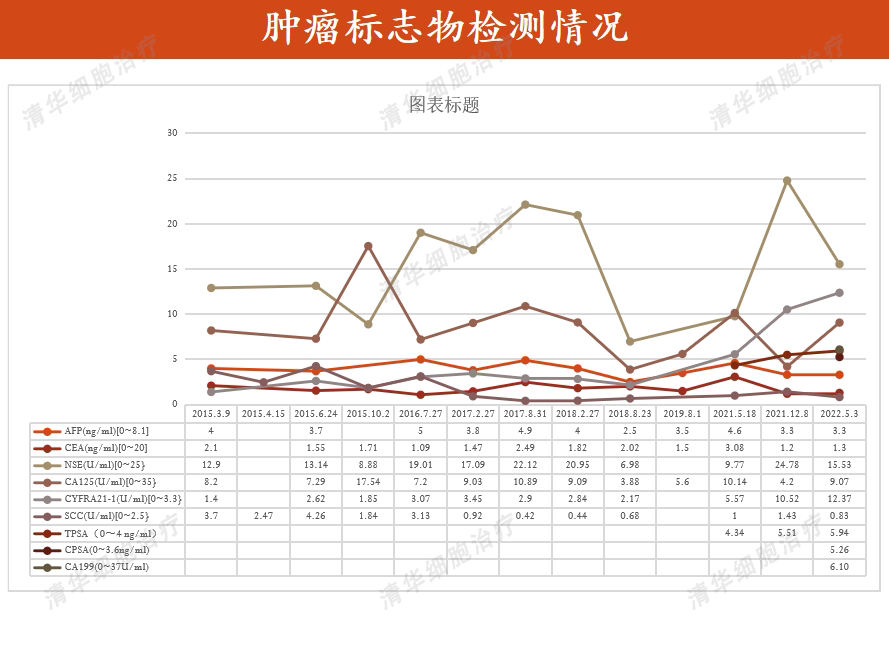
Conclusion and Comments
Click on the image