About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


Overview of the illness
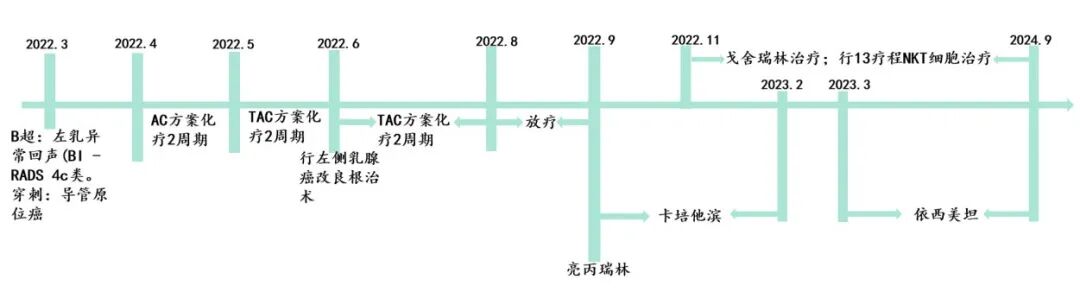
In March 2022, a mass was discovered in the left breast. Half a month later, nipple discharge occurred. On March 20th, a breast ultrasound revealed abnormal echoes in the left breast (BI-RADS category 4c) and enlarged lymph nodes in the left axilla. A left breast biopsy was performed, revealing ductal carcinoma in situ (comprising both acinic and cribriform patterns, high-grade, with visible necrosis) with local infiltration. A left axillary lymph node biopsy was also conducted, and the specimen was found to contain cancer in the connective tissue. On April 1, 2022, a breast MRI demonstrated multiple regional non-mass-like enhancement foci in the left breast, with a BI-RADS score of 5, and enlarged lymph nodes in the left axilla. (Left axillary lymph nodes) invasive carcinoma was detected, accompanied by signet-ring cell differentiation and squamous cell differentiation. Neoadjuvant chemotherapy (FAM-T-E-C-T) was administered on April 9 and 25, 2022.
After surgery, the patient received two courses of TAC chemotherapy (docetaxel + epirubicin + oxaliplatin) on July 14th and August 4th, 2022. On August 3rd, 2022, tumor markers were normal. Radiotherapy was administered on August 25th, September 9th, and September 22nd, 2022. Leuprolide treatment was initiated on September 22nd, 2022. From September 23rd, 2022, to February 24th, 2023, the patient took capecitabine orally. Goserelin treatment was started on November 17th, 2022, and has continued to the present day.
Lehe New Medical [Second Diagnosis and Treatment Suggestion]
2. Chemotherapy has significant side effects and severe damage to the immune system and hematopoietic system, and cannot achieve long-term efficacy, making it an unsatisfactory postoperative adjuvant therapy.
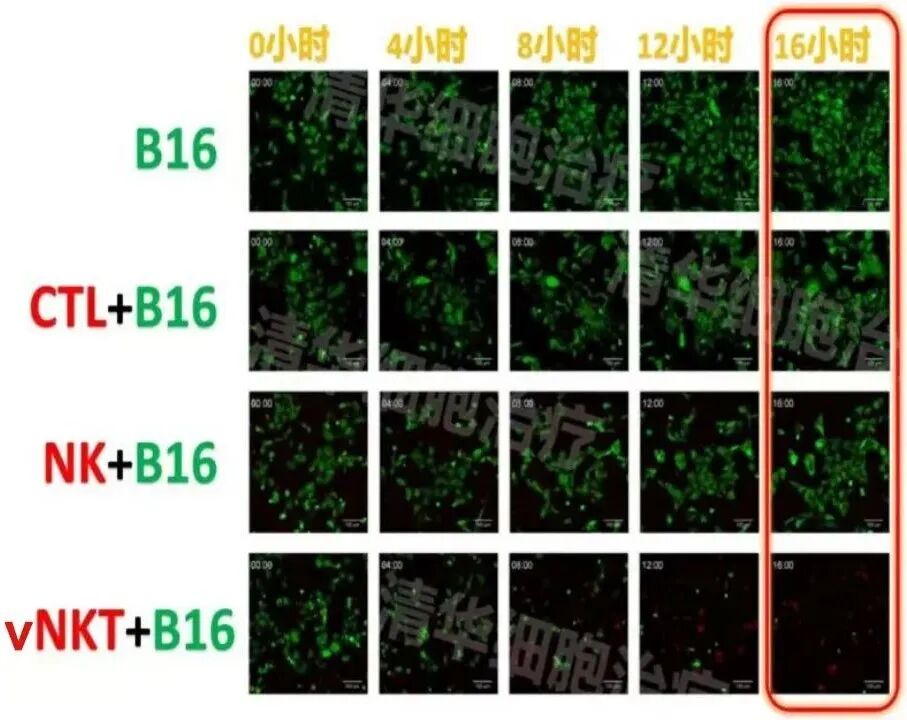
Experimental conditions: In the presence of vNKT cells, after 16 hours, nearly all B16 tumor cells were killed!
Imaging changes
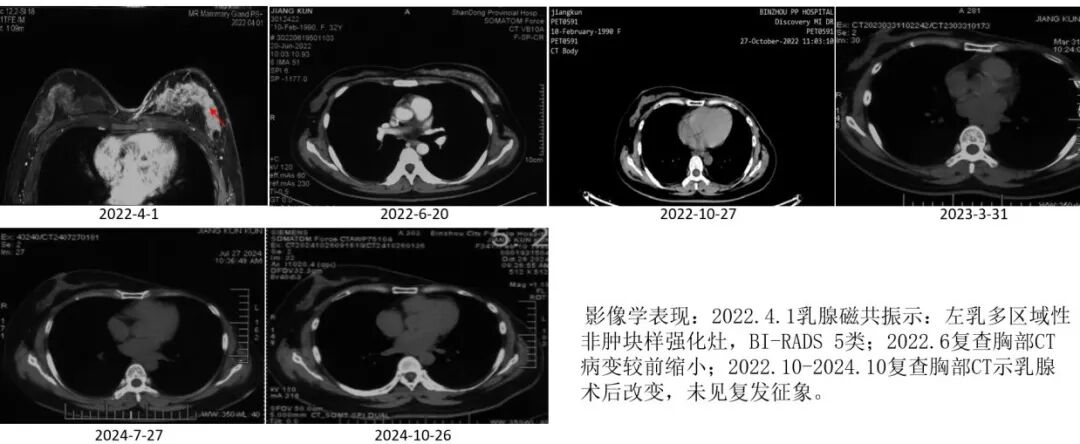
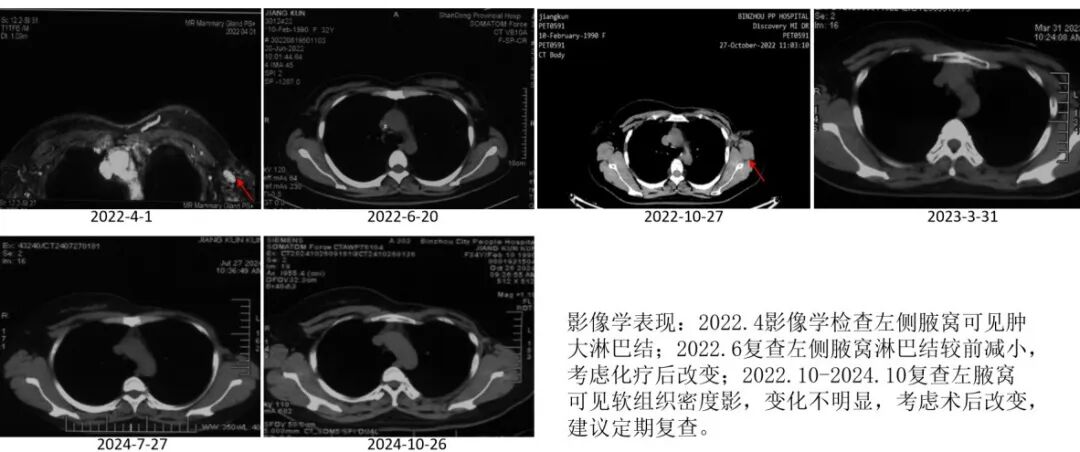
Conclusion and Commentary



Scan QR code
to communicate with Professor Zhang Minghui's team
Click on the image to view past exciting content
