About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。
▲Click on the blue text to follow us
In recent years, immunotherapy has made significant progress in the field of cancer treatment, especially the application of NKT cells (Natural Killer T cells) in anti-tumor immunotherapy, which has received increasing attention. A study published earlier in Frontiers in Immunology showed that iNKT cell therapy has demonstrated encouraging efficacy in lung cancer patients[1]. iNKT cells can recognize the specific antigen α-galactosylceramide (α-GalCer) and rapidly produce a large amount of interferon-γ (IFN-γ), enhancing the tumor-killing ability of NK cells and CD8 T cells.
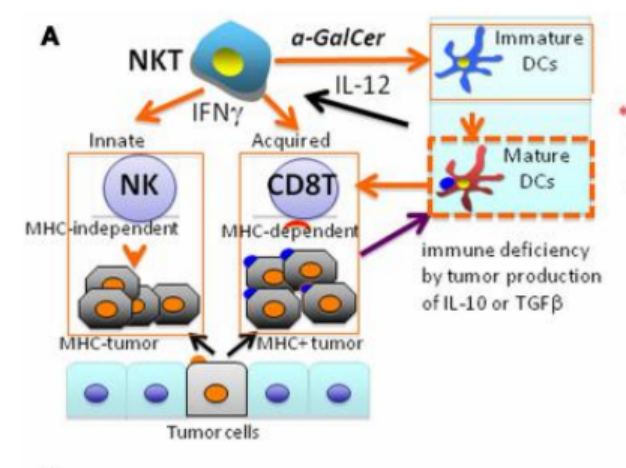
Figure A: Mechanism of NKT Cell-Targeted Helper Cell Therapy
In this study, 17 patients with advanced or recurrent non-small cell lung cancer underwent iNKT+DC cell therapy. The results indicated that 60% of the patients exhibited high expression of IFN-γ, with a significant extension in median survival time to 29.3 months, compared to the median survival time of 4.6 months in the best supportive care (BSC) group (Figure B). This discovery provides compelling evidence for the application of NKT cells in the treatment of lung cancer.
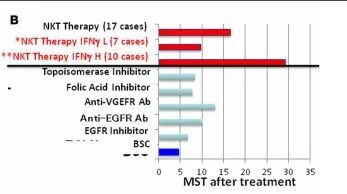
Figure B
Recent research has found[2] that treating NSCLC patients with antigen-presenting cells loaded with iNKT ligands can significantly enhance the number and function of iNKT cells, especially on day 49 after treatment, when a peak in IFN-γ production was observed.This once again suggests that activated iNKT cells play an important role in tumor treatment.Furthermore, the study also points out that changes in the tumor microenvironment may affect the effectiveness of immunotherapy, which means that in future treatments, we need to consider more about regulating the tumor microenvironment.
The vNKT immune cell subpopulation discovered by Zhang Minghui's team at Tsinghua University possesses both the nonspecific recognition function of NK cells and the specific recognition function of CD8+ T cells at the same time,so the dual anti-tumor effect of vNKT cells can rapidly kill tumor cells.It not only directly kills cancer cells, but also kills inhibitory immune cells (Myeloid-derived suppressor cells, MDSCs are a heterogeneous group of cells derived from the bone marrow, which have the ability to significantly inhibit immune cell responses and negatively regulate immune responses.), regulate the microenvironment within cancer tissues, providing new hope for the treatment of solid tumors. At the same time, vNKT cells are collected from the immune cells of healthy individuals, cultured and expanded, and then infused back into patients' bodies, making it easier to achieve treatment.
Tips
Difference between vNKT cells and iNKT cells
iNKT cells (Invariant Natural Killer T cells) and vNKT cells (Variable Natural Killer T cells) are two distinct subpopulations of NKT cells. Currently, the term "NKT cell therapy" commonly used in clinical practice generally refers to iNKT cells. They differ in the diversity and specificity of T cell receptors (TCRs): iNKT cells express a relatively invariant TCRα chain, recognizing specific lipid antigens presented by CD1d molecules. vNKT cells respond to different types of antigens and have more diverse functions, thus exhibiting powerful killing capabilities!
Professor Zhang Minghui explains the difference between vNKT and NKT
Professor Zhang Minghui's research case also confirms the crucial role of vNKT cells in preventing tumor recurrence and metastasis, as well as extending patient survival. Let's showcase the role of vNKT cell therapy in non-small cell lung cancer through a specific case. How can it bring a turnaround to patients in their fight against cancer.
Case Study by Lehe New Medicine Team
Disease Overview
Ms. Wang experienced recurrent coughing and shortness of breath in September 2020. On November 3, 2020, a tracheoscopy was performed to obtain a pathological sample, revealing a "left lower lobe basal branch" suspected to be non-small cell carcinoma. Immediately following, a radical resection of lung cancer was conducted. Postoperative pathology indicated: 1. The left lower lobe and tumor, with a visible tumor adjacent to the lung membrane, measuring 5.5*5*1.3cm in size, and local damage to the lung membrane, covering an area of 1.5*0.5cm, suspected to be intestinal adenocarcinoma; intravascular cancer thrombus was also observed. 2. Metastatic adenocarcinoma of lymph nodes: "Group 10 lymph nodes" (1/2). Immunohistochemistry: TTF-1(-), CK5/6(-), P63(-), ALK(D5F3)(-), ALK(D5F3)Neg(-), TRK(-).
From December 2020 to March 2021, the patient underwent 4 courses of chemotherapy. On July 1, 2022, a thoracoabdominal CT scan revealed multiple enlarged lymph nodes on the lesser curvature of the stomach and in the retroperitoneum, with the most prominent being on the lesser curvature of the stomach (approximately 17x12mm), showing enlargement compared to previous scans and the presence of necrotic areas, suggesting metastasis. On July 15, 2022, the patient underwent exploratory laparotomy, right hemicolectomy, para-aortic lymph node dissection, and splenic hilum lymph node dissection. Postoperative pathology: Metastatic adenocarcinoma of lymph nodes, Group 1, 3, and 7 lymph nodes (1/5), para-aortic lymph nodes (1/1), A mass in the ileocecal junction with a large amount of mucus in the intestinal wall tissue, numerous capillaries were observed within the mucus, and a large number of inflammatory cell infiltration accompanied by granulation tissue reaction were seen around the mucus; focal atypical glandular epithelium was covered, consistent with low-grade appendiceal mucinous tumor, with the lesion located at the opening of the appendix.
Ms. Wang developed abdominal metastasis 1.5 years after surgery, and before fully recovering from the first radical surgery for lung cancer, she underwent exploratory laparotomy to remove the metastatic tumor. These two major surgeries have taken a heavy toll on Ms. Wang, who is 60 years old. If metastasis occurs again, she will not be able to withstand the surgical trauma. To prevent tumor recurrence, after extensive research, Ms. Wang's family sought the help of Professor Zhang Minghui's team at Tsinghua University School of Medicine. After carefully reviewing the demonstration cases of vNKT cell therapy, they particularly hope to terminate tumor progression through treatment.
After carefully reviewing Ms. Wang's medical records, Professor Zhang Minghui provided the following second diagnosis and treatment recommendations:
1. Pathological examination after radical resection of lung cancer revealed the presence of vascular thrombi and lymph node metastasis, indicating that cancer cells had entered the bloodstream and lymph nodes. The abdominal metastasis observed 1.5 years later confirmed this.
2. Pathological examination after exploratory laparotomy indicated lymph node metastasis, increasing the risk of recurrence and metastasis.
3. After undergoing radical resection of lung cancer, chemotherapy, and surgery for abdominal metastasis, Ms. Wang's immune system had been severely compromised. If there were residual cancer cells, they could easily resurge.
4. After surgical removal of tumor burden, timely follow-up with vNKT cell therapy to eliminate residual cancer cells can effectively reduce the incidence of tumor recurrence after surgery.
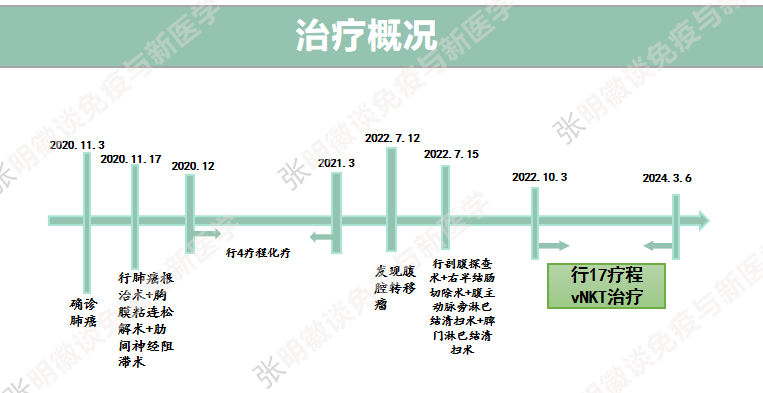
Ms. Wang started vNKT cell therapy on October 3, 2022, and as of March 6, 2024, has undergone a total of 17 courses of treatment. She will continue to receive treatment as planned in the future. After her second metastasis, Ms. Wang did not undergo postoperative chemotherapy and directly proceeded with vNKT treatment. She has now smoothly survived for 2 years and her postoperative survival period has exceeded 4 years, which is a strong proof of the efficacy of vNKT cells. Let's look forward to the follow-up visits.
Imaging changes
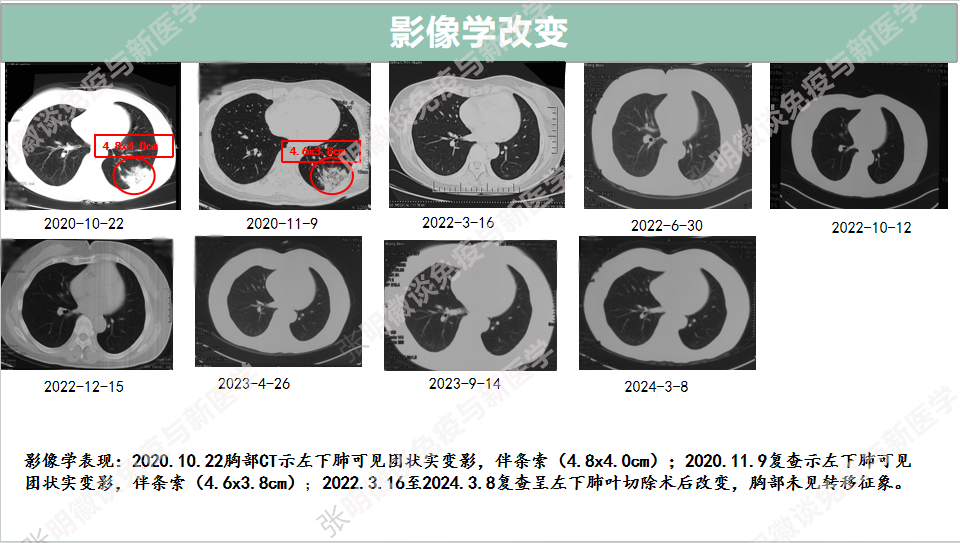
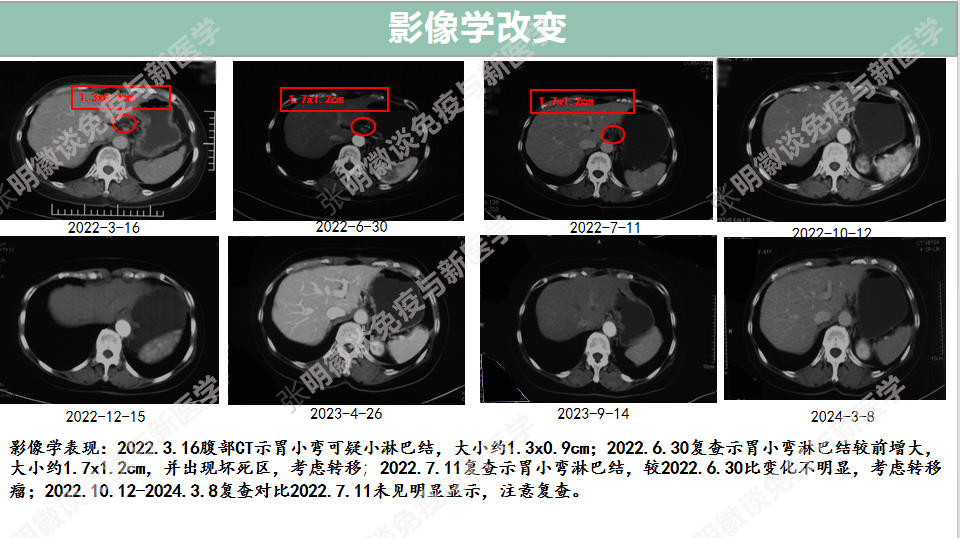
Conclusion and Comments
After receiving vNKT cell therapy, Ms. Wang's quality of life has significantly improved. Not only has her sleep quality greatly improved, but the frequency of colds in autumn and winter has also noticeably decreased. More importantly, she feels more energetic and her daily activities have become easier. This comprehensive improvement in health has filled her with hope for the future.
The importance of postoperative follow-up vNKT cell therapy:
According to the research findings of Zhixing Hao et al., a significant decrease in total lymphocytes, T cells, CD4+ T cells, and NKT cells was observed in the peripheral blood of patients with early-stage NSCLC, which may be related to systemic immune dysfunction and systemic inflammatory response syndrome after surgery[3]. Therefore, postoperative follow-up vNKT cell therapy is particularly important. It can not only replenish the vNKT cells reduced due to disease or surgery but also enhance the body's immune response to tumors by activating the remaining vNKT cells, thereby reducing the risk of recurrence.
Lymph node metastasis is the most common mode of metastasis in lung cancer and an important factor affecting patient staging and prognosis. Firstly, the primary tumor continues to expand, generating new lymphatic vessels, and then malignant tumor cells use these lymph nodes to invade local lymph nodes, causing metastasis to other sites. The lymph node metastasis and vascular cancer thrombus after Ms. Wang's first surgery were risk factors for the second metastasis, and lymph node metastasis still persisted after the second surgery. vNKT cell therapy is a relatively effective treatment method for clearing residual cancer cells and enhancing patient immunity, playing an important role in the patient's own disease treatment intervention.
In summary, the application of vNKT cells in lung cancer treatment not only provides patients with a new treatment option but, more importantly, plays a key role in preventing tumor recurrence. With the continuous advancement of immunotherapy technology, vNKT cell therapy is expected to bring hope to more cancer patients in the future.
References:
[1] Fujii S, Shimizu K, Okamoto Y, et al. NKT cells as an ideal anti-tumor immunotherapeutic[J]. Frontiers in Immunology, 2013, 4: 409.
[2] Iyoda T, Shimizu K, Kawamura M, et al. Augmenting Granzyme B–Expressing NK Cells by Invariant NKT Ligand–Loaded APCs in Patients with Postoperative Early Stage Non–Small Cell Lung Cancer: Results of a Randomized Phase II Study[J]. Immunohorizons, 2023, 7(1): 1-16.
[3] Hao Z, Lin M, Du F, et al. Systemic immune dysregulation correlates with clinical features of early non-small cell lung cancer[J]. Frontiers in Immunology, 2022, 12: 754138.

Contact Us
Scan the QR Code
to communicate with Professor Zhang Minghui's team
Click on the image to view past exciting content
Contributed by: Zhao Tuantuan
Reviewed by: Qiao Jiacheng, Wang Ying, Gao Chen
Edited/typeset by: Zhao Tuantuan
