About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


Overview of the illness
After reviewing Mr. Wang's medical records, Professor Zhang Minghui made the following second diagnosis and treatment suggestion for Lehe New Medical:
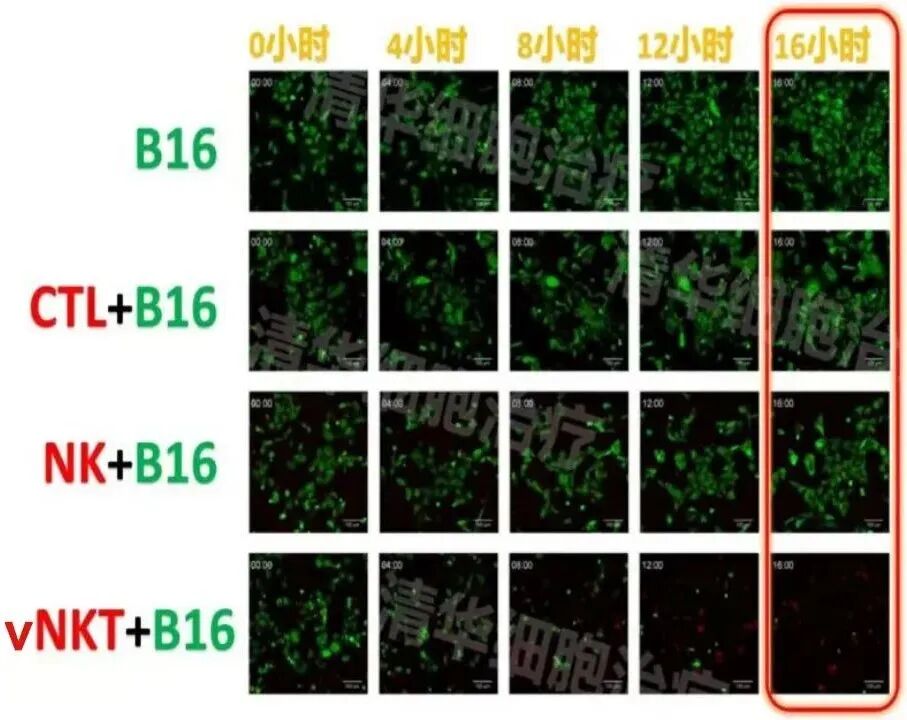
Experimental conditions: In the presence of vNKT cells, after 16 hours, nearly all B16 tumor cells were killed!
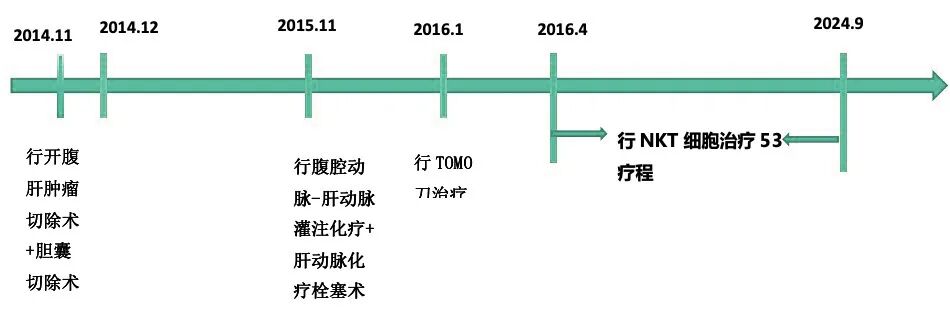
Treatment Experience
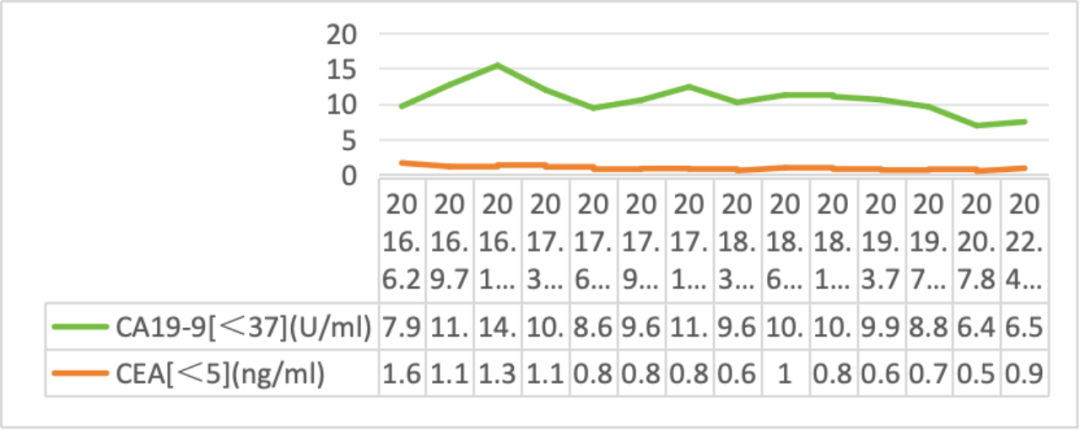
Changes in tumor markers
Imaging changes
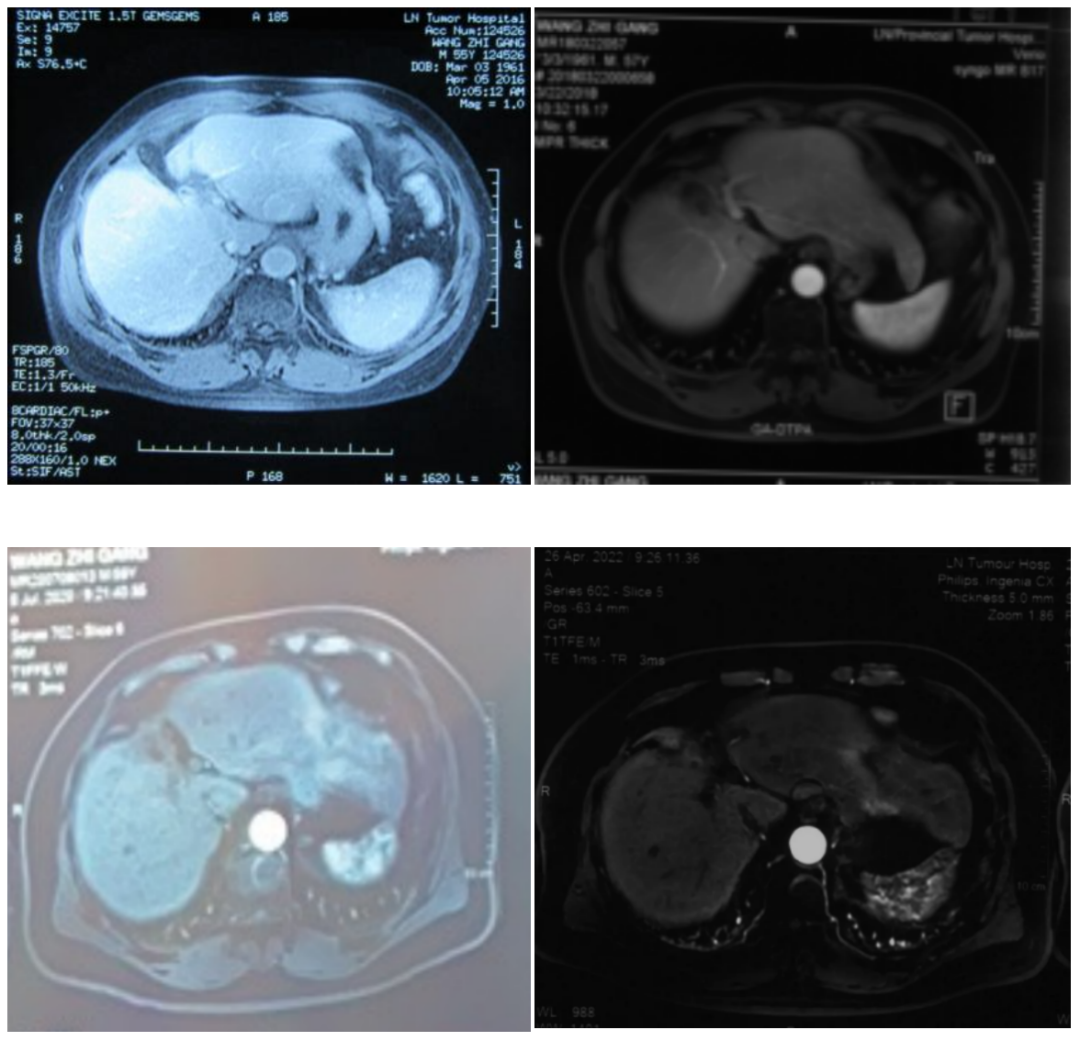
Expert Commentary Cases
Conclusion and Commentary



Scan QR code
Communicate with Professor Zhang Minghui's team

Click on the image to view past exciting content
